


中华护理杂志 ›› 2023, Vol. 58 ›› Issue (7): 822-828.DOI: 10.3761/j.issn.0254-1769.2023.07.008
尹艳茹( ), 周洪昌(
), 周洪昌( ), 刘梦如, 梁发存, 茹运新, 杨文娟, 宁云凤, 丁敏
), 刘梦如, 梁发存, 茹运新, 杨文娟, 宁云凤, 丁敏
收稿日期:2022-05-13
出版日期:2023-04-10
发布日期:2023-04-11
通讯作者:
周洪昌,E-mail:zhouhc529@zjhu.edu.cn作者简介:尹艳茹:女,本科(硕士在读),护师,E-mail:2804398846@qq.com
基金资助:
YIN Yanru( ), ZHOU Hongchang(
), ZHOU Hongchang( ), LIU Mengru, LIANG Facun, RU Yunxin, YANG Wenjuan, NING Yunfeng, DING Min
), LIU Mengru, LIANG Facun, RU Yunxin, YANG Wenjuan, NING Yunfeng, DING Min
Received:2022-05-13
Online:2023-04-10
Published:2023-04-11
摘要:
目的 调查老年维持性血液透析(maintenance hemodialysis,MHD)患者社会隔离现状及影响因素。 方法 便利选取2022年1月—5月湖州市某三级甲等医院230例老年MHD患者,采用一般资料调查表、社会网络量表简表、家庭关怀指数问卷、汉密尔顿抑郁量表、加州大学洛杉矶分校孤独感量表、社会支持评定量表进行横断面调查。将单因素分析具有统计学意义的变量纳入二元Logistic回归进行多因素分析。 结果 230例老年MHD患者社会隔离得分为(12.27±4.44)分,家庭隔离得分为(7.69±1.93)分,朋友隔离得分为(4.58±3.30)分,社会隔离、家庭隔离、朋友隔离发生率分别为45.2%、10.9%、60.4%。二元Logistic回归分析显示,年龄、透析龄、个人月收入、自评健康状况、社会参与、家庭支持、社会支持是老年MHD患者社会隔离的影响因素(P<0.05)。 结论 老年MHD患者社会隔离水平较高,朋友隔离发生率高于家庭隔离。临床医护人员可重点关注年龄大、透析龄长、健康状况差、经济水平低、社会参与少、家庭及社会支持水平低的老年MHD患者,根据相关影响因素制订干预措施,改善老年MHD患者的社会隔离现状,促进身心健康。
尹艳茹, 周洪昌, 刘梦如, 梁发存, 茹运新, 杨文娟, 宁云凤, 丁敏. 老年维持性血液透析患者社会隔离现状的调查研究[J]. 中华护理杂志, 2023, 58(7): 822-828.
YIN Yanru, ZHOU Hongchang, LIU Mengru, LIANG Facun, RU Yunxin, YANG Wenjuan, NING Yunfeng, DING Min. Status and influencing factors of social isolation in elderly patients with maintenance hemodialysis[J]. Chinese Journal of Nursing, 2023, 58(7): 822-828.
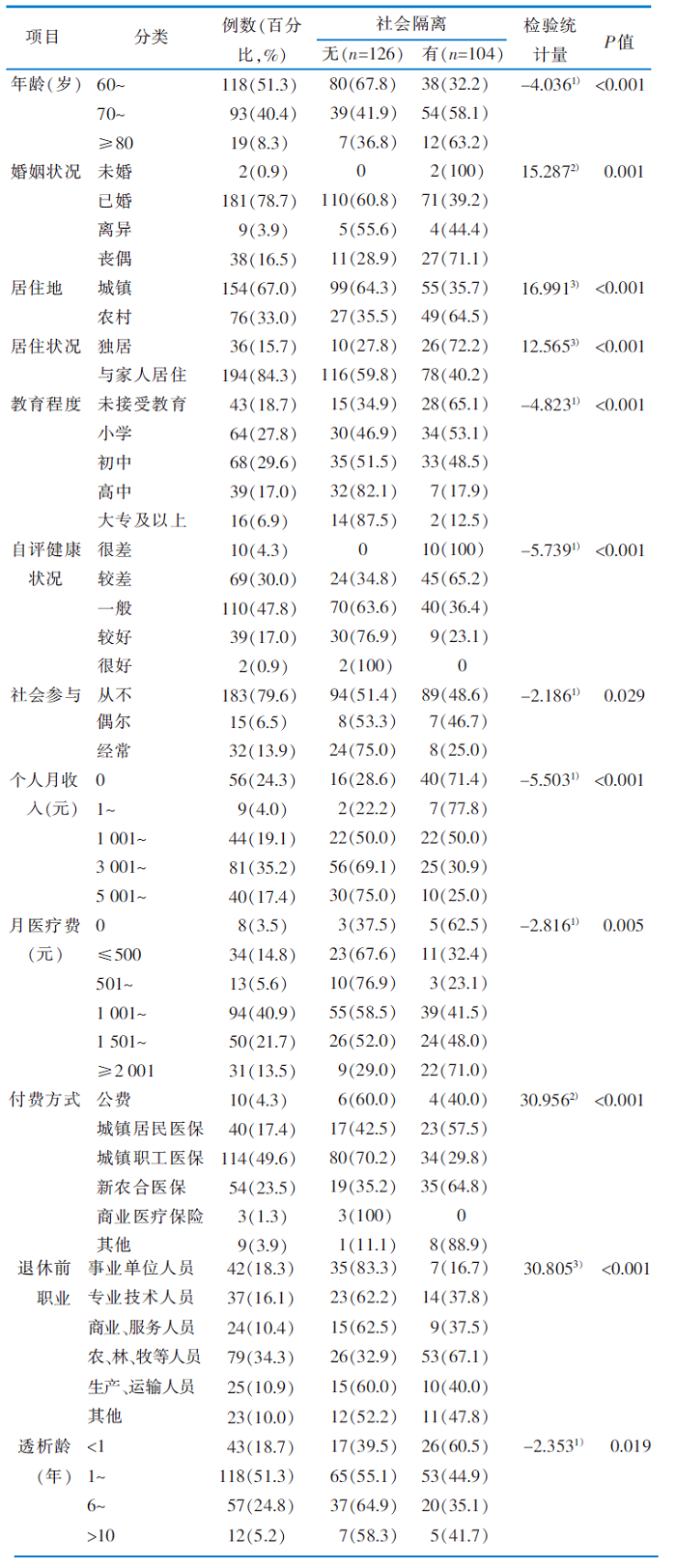 |
表1 调查对象的一般资料和老年维持性血液透析患者社会隔离单因素分析[例(百分比,%)]
Table 1 The general information of the subjects and the univariate analysis of social isolation in elderly maintenance hemodialysis patients[case(percent,%)]
 |
| [1] |
Arhuidese IJ, Beaulieu RJ, Aridi HD, et al. Age-related outcomes of arteriovenous grafts for hemodialysis access[J]. J Vasc Surg, 2020, 72(2):643-650.
DOI PMID |
| [2] |
Coyle CE, Dugan E. Social isolation,loneliness and health among older adults[J]. J Aging Health, 2012, 24(8):1346-1363.
DOI URL |
| [3] | Wu F, Sheng Y. Social isolation and health-promoting behaviors among older adults living with different health statuses:a cross-sectional study[J]. Int J Nurs Sci, 2021, 8(3):304-309. |
| [4] |
del Pozo Cruz B, Perales F, Alfonso-Rosa RM, et al. Impact of social isolation on physical functioning among older adults:a 9-year longitudinal study of a US-representative sample[J]. Am J Prev Med, 2021, 61(2):158-164.
DOI URL |
| [5] | Elovainio M, Lahti J, Pirinen M, et al. Association of social isolation,loneliness and genetic risk with incidence of dementia:UK Biobank Cohort Study[J]. BMJ Open, 2022, 12(2):e053936. |
| [6] |
Brinkhues S, Dukers-Muijrers NHTM, Hoebe CJPA, et al. Socially isolated individuals are more prone to have newly diagnosed and prevalent type 2 diabetes mellitus-the Maastricht study[J]. BMC Public Health, 2017, 17(1):955.
DOI URL |
| [7] |
Santini ZI, Jose PE, Cornwell EY, et al. Social disconnectedness,perceived isolation,and symptoms of depression and anxiety among older Americans(NSHAP):a longitudinal mediation analysis[J]. Lancet Public Health, 2020, 5(1):e62-e70.
DOI PMID |
| [8] |
Yu B, Steptoe A, Chen YJ. Social isolation,loneliness,and all-cause mortality:a cohort study of 35,254 Chinese older adults[J]. J Am Geriatr Soc, 2022, 70(6):1717-1725.
DOI URL |
| [9] | 安嬿. 慢性心力衰竭患者社会隔离现状及其影响因素研究[D]. 济南: 山东大学, 2021. |
| An Y. Social isolation and associated factors in patients with chronic heart failure with chronic heart failure[D]. Jinan: Shan-dong University, 2021. | |
| [10] |
Lubben J, Blozik E, Gillmann G, et al. Performance of an abbreviated version of the Lubben Social Network Scale among three European community-dwelling older adult populations[J]. Gerontologist, 2006, 46(4):503-513.
DOI PMID |
| [11] | Chang QS, Sha F, Chan CH, et al. Validation of an abbreviated version of the Lubben Social Network Scale(“LSNS-6”) and its associations with suicidality among older adults in China[J]. PLoS One, 2018, 13(8):e0201612. |
| [12] | Smilkstein G, Ashworth C, Montano D. Validity and reliability of the family APGAR as a test of family function[J]. J Fam Pract, 1982, 15(2):303-311. |
| [13] | 吕繁, 顾湲. 家庭APGAR问卷及其临床应用[J]. 国外医学(医院管理分册), 1995, 12(2):56-59. |
| Lü F, Gu Y. The family APGAR questionnaire and its clinical application[J]. Foreign Med Sci Ser Hosp Manag, 1995, 12(2):56-59. | |
| [14] | 肖水源. 《社会支持评定量表》的理论基础与研究应用[J]. 临床精神医学杂志, 1994, 4(2):98-100. |
| Xiao SY. The theoretical basis and research application of Social Support Rating Scale[J]. J Clin Psychiatry[J]. J Clin Psychol Med, 1994, 4(2):98-100. | |
| [15] |
Hamilton M. A rating scale for depression[J]. J Neurol Neurosurg Psychiatry, 1960, 23(1):56-62.
DOI URL |
| [16] | 赵靖平, 郑延平. Hamilton抑郁量表的信度和效度[J]. 中国心理卫生杂志, 1992, 6(5):214-216,238. |
| Zhao JP, Zheng YP. Reliability and validity of Hamilton Depression Scale assessed in 329 Chinese depression patients[J]. Chin Ment Heal J, 1992, 6(5):214-216,238. | |
| [17] |
Russell DW. UCLA Loneliness Scale(Version 3):reliability,validity,and factor structure[J]. J Pers Assess, 1996, 66(1):20-40.
DOI PMID |
| [18] | 王登峰. Russell孤独量表的信度与效度研究[J]. 中国临床心理学杂志, 1995, 3(1):23-25. |
| Wang DF. Reliability and validity of the Loneliness Scale[J]. Chin J Clin Psychol, 1995, 3(1):23-25. | |
| [19] | 李少杰, 崔光辉, 尹永田. 社区老年人社会隔离及孤独感对衰弱影响[J]. 中国公共卫生, 2022, 38(4):399-403. |
| Li SJ, Cui GH, Yin YT. Influence of social isolation and loneliness on frailty among community elderly people[J]. Chin J Public Heal, 2022, 38(4):399-403. | |
| [20] |
Al Naamani Z, Gormley K, Noble H, et al. depression and sleep quality in patients undergoing haemodialysis[J]. BMC Nephrol, 2021, 22(1):157.
DOI |
| [21] |
杜晓菊, 张海林, 尹丽霞, 等. 维持性血液透析患者骨骼肌质量下降预测模型的构建及对护理工作的启示[J]. 中华护理杂志, 2021, 56(4):496-501.
DOI |
|
Du XJ, Zhang HL, Yin LX, et al. Establishment and enlightenment of a predictive model for decreased skeletal muscle mass in maintenance hemodialysis patients[J]. Chin J Nurs, 2021, 56(4):496-501.
DOI |
|
| [22] | Zhou WR, Li Y, Ning YC, et al. Social isolation is associated with rapid kidney function decline and the development of chronic kidney diseases in middle-aged and elderly adults:findings from the China health and retirement longitudinal study(CHARLS)[J]. Front Med(Lausanne), 2021, 8:782624. |
| [23] | 赵迪. 社区老年人社会隔离现状及对生活质量的影响机制研究[D]. 青岛: 青岛大学, 2021. |
| Zhao D. Study on the status of social isolation and its influence mechanism on the quality of life in community-dwelling older adults[D]. Qingdao: Qingdao University, 2021. | |
| [24] |
Child ST, Lawton L. Loneliness and social isolation among young and late middle-age adults:associations with personal networks and social participation[J]. Aging Ment Health, 2019, 23(2):196-204.
DOI URL |
| [25] |
Moorthi RN, Latham-Mintus K. Social isolation in chronic kidney disease and the role of mobility limitation[J]. Clin Kidney J, 2019, 12(4):602-610.
DOI PMID |
| [26] | Silva P, Matos AD, Martinez-Pecino R. The contribution of the Internet to reducing social isolation in individuals aged 50 years and older:quantitative study of data from the survey of health,ageing and retirement in Europe[J]. J Med Internet Res, 2022, 24(1):e20466. |
| [27] | 翟春城, 段卉, 石杰, 等. 农村居民社会隔离对生存质量的影响:经济状况的调节作用[J]. 中国卫生事业管理, 2018, 35(12):923-925. |
| Zhai CC, Duan H, Shi J, et al. Studying on the influence of social isolation on the life quality of rural residents regulated by economic conditions[J]. Chin Heal Serv Manag, 2018, 35(12):923-925. | |
| [28] | 韩影, 刘瑶, 许丽雅, 等. 家庭关怀及社会支持对社区老年人社会隔离的影响[J]. 现代预防医学, 2020, 47(9):1612-1616. |
| Han Y, Liu Y, Xu LY, et al. Family care and social support on social isolation of the elderly in community[J]. Mod Prev Med, 2020, 47(9):1612-1616. | |
| [29] | 张翠霞, 余秀峰, 吴云霞, 等. 社会支持干预对提高维持性血液透析患者生活质量[J]. 中国健康心理学杂志, 2018, 26(11):1622-1625. |
| Zhang CX, Yu XF, Wu YX, et al. The effect of social support intervention on improving the quality of life of maintenance hemodialysis patients[J]. China J Heal Psychol, 2018, 26(11):1622-1625. | |
| [30] |
Heffernan E, Withanachchi CM, Ferguson MA. ‘The worse my hearing got,the less sociable I got’:a qualitative study of patient and professional views of the management of social isolation and hearing loss[J]. Age Ageing, 2022, 51(2):afac019.
DOI URL |
| [1] | 郭员志, 张红梅, 赵培, 王琦, 李玉环, 王淑芬, 于洋. 乳腺癌术后淋巴水肿预防与护理的循证实践[J]. 中华护理杂志, 2023, 58(7): 773-780. |
| [2] | 武佩佩, 王盈, 沈傲梅, 强万敏, 杨惠莉, 刘鑫鑫. 乳腺癌相关淋巴水肿患者综合消肿治疗依从性的质性研究[J]. 中华护理杂志, 2023, 58(7): 781-787. |
| [3] | 何丽, 胡露红, 崔金锐, 邓妍, 褚彦香, 王玮荻, 王倩云. 乳腺癌化疗患者自我倡权能力现状及影响因素分析[J]. 中华护理杂志, 2023, 58(7): 788-793. |
| [4] | 刘英, 甄倩, 王晓庄, 张皎霄, 张亚平, 王德欣, 王熙棋. 乳腺癌患者和配偶的创伤后成长及与积极心理资本的关系[J]. 中华护理杂志, 2023, 58(7): 794-799. |
| [5] | 吴媛, 张玉玺, 王楠楠, 张慧超. 乳腺癌患者参与同伴支持体验质性研究的Meta整合[J]. 中华护理杂志, 2023, 58(7): 800-807. |
| [6] | 荆凤, 王园园, 邢唯杰, 徐蕾, 胡雁. 乳腺癌患者芳香化酶抑制剂诱导的骨关节症状预防和管理的证据总结[J]. 中华护理杂志, 2023, 58(7): 808-815. |
| [7] | 周彦君, 李秋月, 胡宇乐, 杨浩杰, 赵芳, 梁涛. 乳腺癌蒽环类化疗相关心脏毒性早期识别及预防的研究进展[J]. 中华护理杂志, 2023, 58(7): 816-821. |
| [8] | 何雯倩, 郭园丽, 王连珂, 周乾宇, 王盼盼, 张配嘉, 赵明扬, 王荣荣, 要子慧, 胡博, 吴田田, 王昱, 孙长青. 首发脑卒中患者护理依赖轨迹的潜在类别及影响因素分析[J]. 中华护理杂志, 2023, 58(7): 829-835. |
| [9] | 李琴, 刘婷, 张珊, 燕菊, 张嫣然, 苗秀欣. 痛风患者疾病感知评估量表的编制及信效度检验[J]. 中华护理杂志, 2023, 58(7): 836-842. |
| [10] | 余舒欣, 林荣, 祝雪花. 政策工具视角下国内护理卫生政策的文本分析[J]. 中华护理杂志, 2023, 58(7): 843-849. |
| [11] | 胡鹏, 李琴, 杨媛, 黎海阳, 张成娟, 雒敏. “护士银行”模式短期效应的实证研究[J]. 中华护理杂志, 2023, 58(7): 850-856. |
| [12] | 谢琼华, 骆尹, 郝富杰, 姜懿珊, 郭爱敏. 慢性阻塞性肺疾病患者家庭呼吸康复护理的最佳证据总结[J]. 中华护理杂志, 2023, 58(7): 857-863. |
| [13] | 马喜宁, 白艳娟, 孔思铭, 黄蓉, 张静, 姚辉. 强直性脊柱炎患者运动指导方案的最佳证据总结[J]. 中华护理杂志, 2023, 58(7): 864-870. |
| [14] | 严露培, 刘丽, 胡秀英. 派生策略在护理领域中的研究进展[J]. 中华护理杂志, 2023, 58(7): 871-874. |
| [15] | 李志茹, 王华芬, 卢芳燕, 吕璐洋, 鲍瑞洁, 董丽. 肝移植受者从青少年到成人过渡期准备的研究进展[J]. 中华护理杂志, 2023, 58(7): 875-880. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||